- posted: Jan. 06, 2017
Don’t have a night of eczema like the HBO hit show The Night Of!
http://www.youtube.com/watch?v=qaU5Rl_dndA
Caring for Eczema in Winter
A chronic skin condition like eczema can be challenging during the cold winter months. Eczema becomes worse during the winter months due to the extreme temperatures. Typically eczema is seen as flaky patches of skin. If you suffer don’t stress; it can be effectively calmed and reduced with the right types of skin care.
What is Eczema?
Eczema, sometimes referred to as dermatitis, is a cluster of skin conditions that have varying symptoms, the most common of which is dry skin. Normal skin produces oils that create a barrier to prevent water loss and stop irritants from penetrating the skin. If you have eczema, your skin does not do this as effectively. Eczema, has a wider range of symptoms. It’s also a chronic skin condition and it often has redness, swelling, itching, dryness, rashes and more. While the cause is unknown, symptoms can be triggered by the use of certain skin care products and environmental conditions, especially the drying conditions frequently experienced during cold, windy winter months.
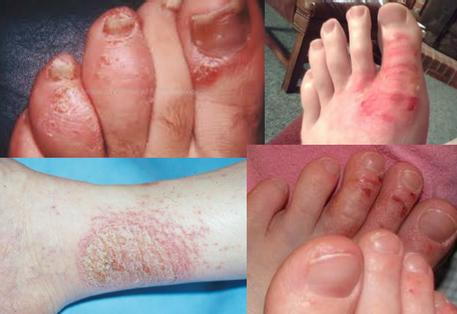
Here are the various types with their symptoms:
Atopic Eczema: Dryness, itchiness (pruritus), redness, inflammation. If infected, skin may crack and weep.
Allergic Contact Dermatitis: Dry, itchy skin; redness, inflammation, rash, or blistering.
Irritant Contact Dermatitis: Itchy, dry skin; rash—usually on hands but can be seen on feet due to irritation from sock or materials in shoes.
Varicose (Asteatotic) Eczema: Affects the lower legs. Appears on the skin around the shins and ankles. Skin is itchy, inflamed and speckled. Ulcers can occur.
Discoid (Nummular) Eczema: Coin-shaped, reddened area. Normally appears suddenly on lower legs or trunk. Can be itchy and weep fluid.
What Causes This?
In atopic eczema, the most common form of eczema, the exact cause is unknown, but it is generally thought that people inherit a tendency toward the disorder. People with atopic eczema are generally sensitive to allergens in the environment that others find harmless. It is also closely linked with asthma and hay fever. The symptoms can be set off by a number of triggers.
In Allergic Contact Dermatitis, the immune system responds to a substance that comes in contact with the skin. Common allergens include poison ivy and oak, nickel and other metals, perfume, sunscreens, rubber.
In Irritant Contact Dermatitis, the cause is contact with everyday substances, such as bleaches, caustic detergents, chemicals, soap. Exposure to tar or certain plant juices, including celery, lime, and parsley, in conjunction with light can cause phototoxic reaction.
Varicose (Asteatotic) Eczema can be the result of poor venous circulation.
Discoid (Nummular) Eczema has no known cause and is associated with dry skin that worsens in dry weather.
How Winter Months affects Eczema?
Eczema is often experienced only in the fall and winter. This is due to the drying effects of the season. Cold winds on exposed skin can aggravate the condition. Strong heat in buildings and at home can cause dryness of the skin.
Best Product Ingredients for Winter Months
For those who prone to eczema flare ups, especially during the winter, it is important to use products that will not only moisturize and heal the skin, but also contains ingredients that will be less likely to trigger a negative reaction or flare up.
Chamomile can reduce symptoms of eczema, promote healing, and moisturize the skin. It is also good for anyone with sensitive skin.
Witch hazel is both antiseptic and moisturizing and is beneficial after cleaning and before moisturizing to minimize the risk of infection. Witch hazel can be soothing to skin that is itchy or irritated. Try using a moisturizer with witch hazel to soothe skin daily.
By using the right products and being aware of the best ingredients to use, those with eczema can easily minimize the effects that winter has on these conditions. Listen to Your Body
Healing Alternatives
As with dry skin, the first line of treatment against eczema is emollient therapy. When emollients are used correctly, mild to moderate symptoms of eczema can be controlled without having to resort to stronger measures, such as steroids.
Many doctors recommend steroids to control severe symptoms. While steroids can dramatically improve the condition, there can also be a rebound inflammatory response when they are discontinued. Hydrocortisone cream is a topical steroid that is available over the counter without a prescription. It is one of the weaker steroid creams. You may want to try this before resorting to prescription-strength steroids. I do not recommend steroid use for long periods of time.
Antihistamines can also help relieve itching and may help you get some sleep, but again, I do not recommend ongoing reliance on these. Some eczema sufferers have also successfully used light therapy. Ask your doctor if either of these are good short-term therapies for your eczema; caution should be exercised with exposure to light, as some dermatitis conditions are photosensitive.
The following are standard treatments for the various types of eczema:
Atopic Eczema: Emollients, topical steroids, behavior modification.
Allergic Contact Dermatitis: Prevent contact with allergen. Use topical ointments or steroid creams.
Irritant Contact Dermatitis: Avoid irritants, keep skin moisturized.
Adult Seborrheic Eczema: Anti-fungal shampoos and creams.
Varicose (Asteatotic) Eczema: Emollients, steroid creams.
Discoid (Nummular) Eczema: Emollients, steroid creams.
Here are some steps you can take to make the condition less aggravating:
Keep a positive attitude: Negative emotions start a hormonal cascade that can trigger or worsen your symptoms.
Wear natural fabrics: Cotton and other soft, natural fabrics can limit irritation. Avoid wool and synthetic fabrics.
Do not scratch: Scratching can lead to infection.
Reduce household irritants: Try to get rid of dust, dust mites, fur and dander from pets by vacuuming often, using air filters and keeping your house clean. You may also want to use anti-allergenic bedding.
Use gentle washing powders: Avoid harsh detergents and scented cleansers.
Try relaxation therapy: Relaxation therapy and massage therapy modalities can help by reducing muscle tension. This can lead to less aggravation and other detrimental psychological factors that contribute to flare ups.
Keep your bedroom cool: Overheating aggravates itching. So does dry air. You may want to use a humidifier or keep a saucer of water in each room to keep moisture in the air. If you heat with a woodstove, place a kettle of water on top to release steam and check it often.
Locations
Hours of Operation
9:00 am - 5:00 pm
9:00 am - 5:00 pm
9:00 am - 5:00 pm
9:00 am - 5:00 pm
9:00 am - 5:00 pm
By Appointment
Closed
