More About Toe Nail Fungus
- posted: Mar. 13, 2017
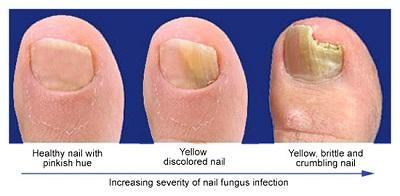
Toenail Fungus Cause Treatment and PreventionNail Fungus (Onychomycosis) Thickened, brittle, discolored and often painful nails are often caused by a fungal infection of the nail. This condition can occur for a Read More
Acupuncture and Foot Pain
- posted: Mar. 23, 2017
Acupuncture has been used for thousands of years to treat many diseases, chronic conditions and acute symptoms. It can be particularly beneficial for pain, as it can treat both locally Read More
Ingrown Toenail - Treat & Prevent
- posted: May 01, 2017
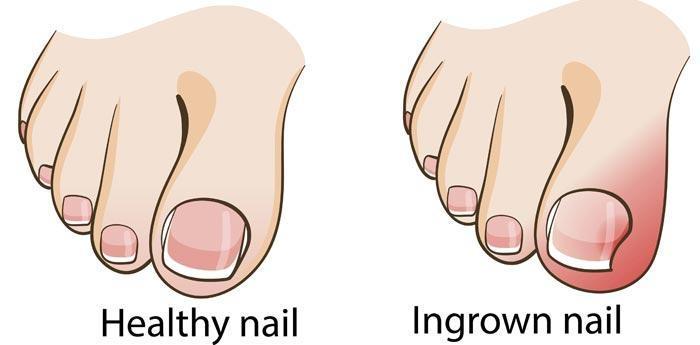
Ingrown Toenail - How to Treat and Prevent Ingrown toenails, medically known as onychocryptosis, usually is caused by trimming toenails too short. Specifically, the area on the sides of the big Read More
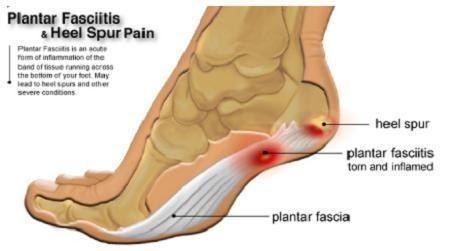
New Non-Invasive Heel Pain Treatment at the Jersey Shore
- posted: Jun. 07, 2017
Many people have so many questions and concerns when considering treatment options for heel pain. New non-invasive heel pain treatment with EPAT brings many questions by patients at our Jersey Read More
Heel Pain Treatment: PRP vs. Steroid Injection
- posted: Jun. 26, 2017
HEEL PAIN TREATMENT:PRP VS. STEROID INJECTIONS Steroid injections have been around what seems like forever but platelet rich plasma (PRP) has been the new latest craze in heel pain treatment in Read More
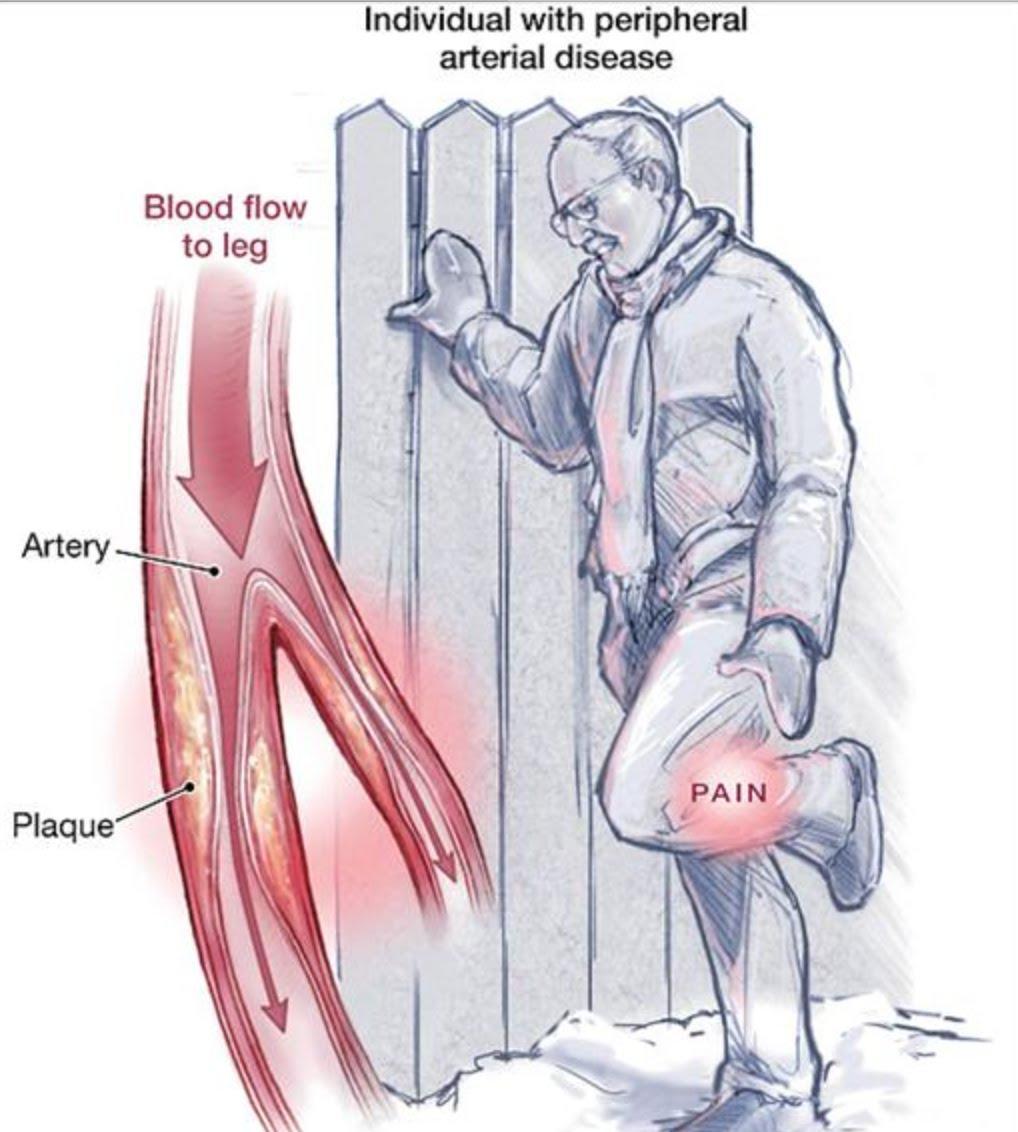
Peripheral Arterial Disease (PAD)
- posted: Sep. 13, 2017
September is Peripheral Arterial Disease ( P.A.D.) Awareness Month! Vascular Access Centers of Eatontown, is offering PAD Screening at No Cost all Month!Here are some interesting facts about Peripheral Arterial Disease Read More
Doctor Recommended Best Baby Shoes
- posted: Oct. 04, 2018
An Excellent Choice for a Soft Sole Crib Shoe My baby had been barefoot for the first few months aside from socks on occasion to go out. Looking back, I probably Read More
Shoes For The Newly Walking Baby
- posted: Oct. 18, 2018
My baby just started walking what shoes are Best! There are so many options for new walker shoes how do you choose? As a podiatrist who treats pediatric patients I find Read More
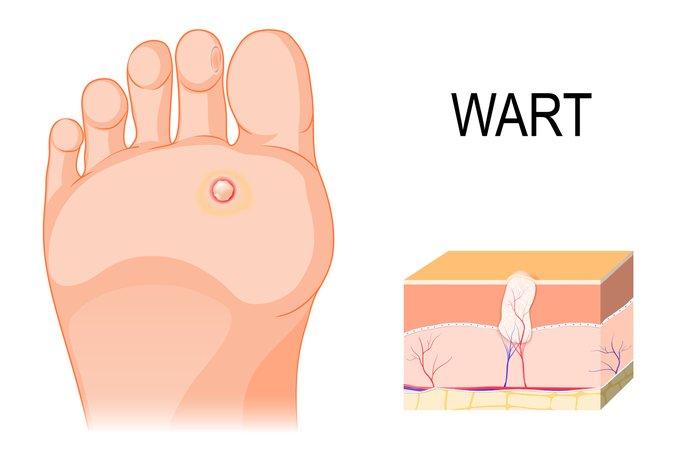
Do I Have A Wart On My Foot!
- posted: Jul. 17, 2019
What are Warts? Warts are one of several soft tissue conditions of the foot that can be quite painful. They are caused by a virus and can appear anywhere on the Read More
Locations
Hours of Operation
9:00 am - 5:00 pm
9:00 am - 5:00 pm
9:00 am - 5:00 pm
9:00 am - 5:00 pm
9:00 am - 5:00 pm
By Appointment
Closed